Is dental nursing a pain in the neck?
Published: 23/10/2020
Dental nurse Preetee Hylton stands up for patient care, while Mary Kristy offers some exercises to mitigate those health risks
Throughout my career, I have never had a chair as a dental nurse and still don't. This isn't because the No8 Partnership, the practice where I work in London's Chelsea, has not provided me with one; it is simply because I refuse to sit when working – unless I am tapping away on the keyboard during six-point periodontal charting or consultations.
As a reader, you must have now realised this article is going to be about aches and pains related to the dental profession – mainly the dental nurses. Here are some key thoughts on the topic:
1. I was not trained as a dental nurse to help patients and clinicians whilst sat on a chair.
2. I have worked in small surgeries in the past, where the dentist can barely move, leaving little to no space for a dental nurse chair. If there was one, it was mainly used for patients to rest their bags and coats. Ergonomics has been an issue as some surgeries are poorly designed.
3. There are practices where sterilised instruments are stored in a separate area or where various surgeries share one specific container of material. This has had me running all over the premises, leaving no time to sit down and get up repetitively.
4. The disparity in height between colleagues matters. You may chuckle at this but my work partner, John Good, is 1m 89cm and I am a mere 1m 63cm. We are only at equal height when he is sat on his chair and, for me, it is less challenging to fulfil my duties in assisting both my clinician and the patient as a dental nurse when on my feet.
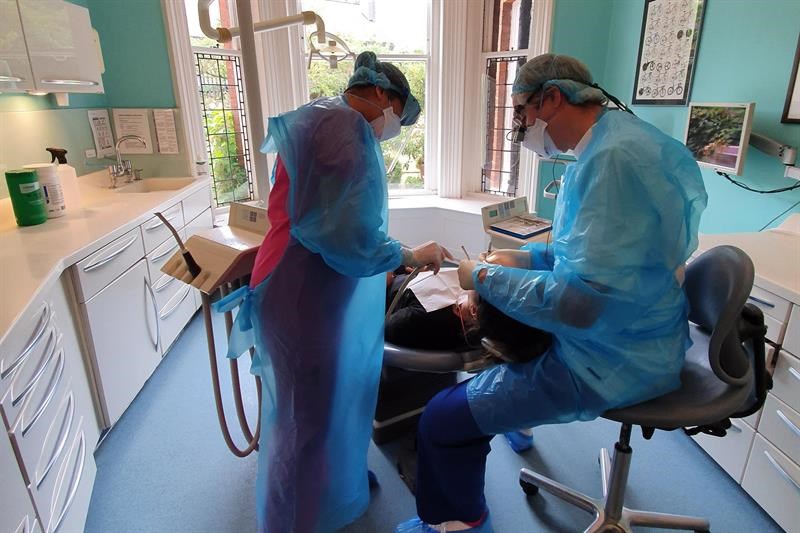
5. I spend hours standing, and sometimes have to remain in the same (often awkward and strained) position for prolonged periods of time during lengthy treatments – especially during restorative and surgical procedures.
Common complaints
I am certain a few of the points mentioned above apply to most dental nurses in the profession.
Low back pain is indeed a common complaint among us – this may vary from a mild feeling of stiffness to obvious, sharp pulsating pain. Another common problem is neck and shoulder ache, mainly stemming from psychosocial factors. Dentistry is known to be stressful and the current situation with COVID-19 has contributed to this.
Mary Kristy has very kindly collaborated with Dental Nursing Academy and hosted a webinar in June, which included a demonstration of exercises that could be carried out during breaks at work – something which she shall elaborate on in this article.
While there is greater awareness of musculoskeletal disorders within the profession, there is still a high prevalence of lower back and neck pain among us.
The use of dental loupes has improved posture in dentists, general and specialists alike, due to having a specific focal length; I understand that some universities have introduced yoga as part of the curriculum for dental students.
Unfortunately, the same cannot be said for the support of dental nurses. There is currently an ongoingdiscussion with management about a similar process for our dental nursing students, which we believe would be invaluable. By having monthly discussions, we intend to increase awareness of the potential problems and support our students in relation to skeletal disorders.
However, good habits start from the very first day of practical training at the work placement – for all dental professionals. Any physical discomfort experienced while working in the clinical environment must be communicated clearly to management to find a solution and mitigate the risk of further injury.
In the past, most dental nurses tended to focus solely on the comfort of their clinicians and their patients, neglecting their own health. There is now more awareness of MSDs, leading to us seeking support and treatment from professionals like Mary Kristy...
Q&A with PT Mary Kristy…
What can dental nurses do to protect themselves physically as they return to work?
- Have regular breaks to allow the tissues and joints to recover from potential strain caused by repetitive movements, techniques and use of equipment.
- Make use of your breaks to do movements that counter your working posture. Check your ergonomics (work environment and set up, such as the patient’s chair height, equipment table accessibility and lighting.
- Consider and discuss with managers a realistic return to work regarding intensity, expectations and hours. Like an athlete, you cannot expect to be at the peak of your performance for competition after two months without training.
- Keep active and moving outside work. Online exercise sessions, such as yoga, Pilates, personal trainers and sports an all help. If you have not been active during your time off, proceed with caution going back to work, or when starting sports.
- Get your regular physical capacity checked with a physiotherapist, chiropractor, osteopath personal trainer or massage therapist. It’s no different to the way you recommend that patients have an annual or biannual dental check and maintenance.
If you have had a history of conditions previously or have paused a physiotherapy management programme during the lockdown times, please resume your programme and have adequate follow up.
What are the common physical problems regarding repetitive activities at work?
The main global condition that comes from literature research is low back pain, followed by upper limb and back repetitive strain injuries. Note, however, those two are umbrella terms for describing general problems , and are not diagnosis.
Back and shoulder pain – what exercises do you recommend as a preventative measure?
Dentists and dental professionals encourage patients to brush and floss teeth, yet still need assess every individual case for a tailored management. It is the no different from a physiotherapist's perspective.
Yoga, Pilates, clinical Pilates, gym group classes, personal training and even cross-fit sessions are the generic recommendations. However, some individuals may need a more rigorous assessment to test safety to work out and may require a tailored programme to meet their physical levels and requirements for their work demands.
What are the symptoms of musculoskeletal disorders?
The most common symptoms are:
- Pain
- Stiffness
- Weakness
- Loss of function
- Pins and needles, and/or numbness.
How important is it to maintain good posture and good fitness as a dental nurse?
‘Bad’ posture may cause problems when done in high repetitions or under load or for prolonged periods of time.
‘Good’ posture is what is considered neutral and optimal for movement. Dentistry is a physically demanding job, therefore movement optimality should always be a priority. Maintaining a good posture should not come from a mental conscious command, rather, it should come from muscle memory and trained habit origin. This is why exercises, weight or resistance training, and clinical Pilates, done with a PROPER TECHNIQUE are extremely important for any physical worker.
How important is it to get into good habits and work with a dentist to ensure comfort for both?
Ideally, every dental clinic should have a physio/occupational therapist or similar ergonomic professional to assess the environment for every new member of staff. They should also recommend a set of tailored exercises to help assist the new staff member if there’s any discrepancy.
Any fitness equipment you can recommend?
I am a big fan of TheraBand resistance bands, or exercise bands, as they are light to pack. As a traveller and sports addict, these are so handy on the go, when doing a cheeky set of exercises on holiday or during my breaks at work. Second on the list, I find myself always looking for a foam roller to self-massage and to release my tight muscles and spinal joints – again, these are great when travelling. I prefer a long foam roller instead of a short one, as it can be used for stabilisation and strengthening exercises as well.
How are you collaborating with Preetee on Instagram?
We have been discussing the physical demands and issues that dental professionals endure on a regular basis and this has prompted me to do short and simple movement videos on my Instagram page (theaussie_pt) and share it with the Dental Nursing Academy. My goal is to help the dental profession keep safe, healthy and active. Physiotherapy and dentistry are physically demanding professions – and, without physical fitness, our ability to perform optimally for the best outcome for our patients can be hampered.
Do you find social media a great way to engage and connect?
Definitely. I joined Instagram last year and I love how short and quirky posts can help convey messages and connect with people of the same community and interest. At first glance, my Instagram page may look a little chaotic as it is primarily my personal account but, increasingly, I am posting more physiotherapy-relevant content as it has become such an important part of my life and a great way to share key messages with my followers.
Author: Preetee Hylton










.jpg?width=150&height=100&scale=canvas)